Shingles is caused by the chickenpox virus (varicella-zoster virus).1 It is characterised by a band of blistering, painful, rashes appearing on the body that lasts for 2-4 weeks.2 Although most individuals recover fully from shingles with treatment, some experience complications that can last for months or even years, most common being persistent nerve pain at the affected site (called postherpetic neuralgia; PHN).3
Any individual who has had chickenpox or been exposed to the chickenpox virus can get shingles.1

What increases your risk of shingles?
AGE: The most important risk factor for shingles is ageing. Shingles most commonly occurs in individuals 50 years and older.2
Why does age matter?
As we age, our immune system weakens. This is a natural process and is called age-related decline in immunity.3 This can allow the usually inactive chickenpox virus to reactivate, causing shingles even though we may feel healthy. In fact, both the risk of shingles and the risk of complications of shingles increases with age.2 This is why, individuals ≥50 years old are encouraged to discuss prevention of shingles with their doctor.1,2
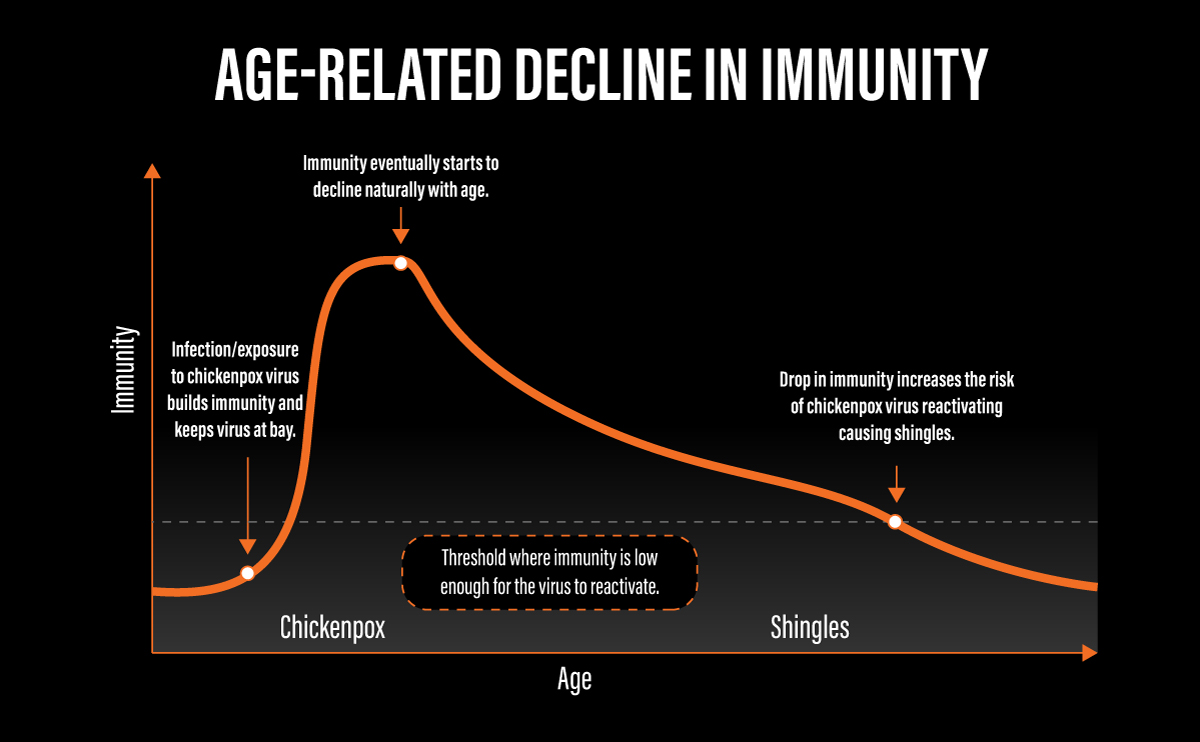
Timeline illustrating how age-related decline in immunity increases the risk of shingles3,5
CHRONIC DISEASES: Diabetes, heart disease, asthma, chronic lung disease and chronic kidney disease can also negatively impact the immune system. This makes individuals living with these conditions at an added risk of developing shingles, on top of their age.3,6
STRESS: Individuals who have recently undergone surgery or experience high levels of emotional or psychological stress are at higher risk of developing shingles.3,6
OTHER INFECTIONS: Co-existing infections (e.g. HIV) or recent recovery from infections (e.g. COVID-19) increases the risk for developing shingles.6,7
FAMILY HISTORY: Those with a family history of shingles (first-degree relatives) are also at higher risk of developing shingles.6
WEAKENED IMMUNE SYSTEM: Individuals who are immunocompromised as a result of a known disease or who are taking medications that suppress the immune system, such as anti-cancer drugs or high-dose steroids, are at higher risk of developing shingles.3
Try the Shingles Risk Test to determine your risk and speak to your doctor about shingles prevention.

- Centers for Disease Control and Prevention. Herpes Zoster (Shingles). Available at: https://www.cdc.gov/shingles/hcp/clinical-overview.html. Accessed May 2022.
- Centers for Disease Control and Prevention (US). Morbidity and Mortality Weekly Report. Prevention of Herpes Zoster. Available at: https://www.cdc.gov/mmwr/preview/mmwrhtml/rr5705a1.htm. Accessed May 2022.
- Chen L-K, et al. BMC Infect Dis. 2017; 17:213. doi: 10.1186/s12879-017-2198-y.
- Fatha N, et al. Int J Infect Dis. 2014;22:73-77.
- Kimberlin DW, Whitely RJ. N Eng J Med. 2007;356:1338-1343.
- Marra F, et al. Open Forum Infect Dis. 2020;7(1):ofaa005. doi: 10.1093/ofid/ofaa005.
- Bhavsar A, et al. Open Forum Infect Dis. 2022. doi: 10.1093/ofid/ofac118.
- GSK is not responsible for third-party website content.



